Gingivitis is characterized by red and swollen gums that bleed easily. It can also lead to periodontitis, a more severe gum disease.
Gingivitis can usually be reversed by visiting a dental professional and practicing good oral hygiene at home. However, gingivitis can also be caused by medications like phenytoin (used for epilepsy), Dilantin (used for angina), and vitamin deficiencies. Click https://bocadentallasvegas.com/ to learn more.
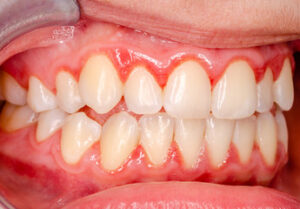
Gingivitis is the earliest stage of gum disease (periodontitis). When left untreated, gingivitis can lead to more serious gum diseases such as periodontitis, which can cause bone loss and tooth loss. Gingivitis is caused by the buildup of plaque — a sticky film that contains bacteria — on teeth and gums. The bacteria in plaque produce toxins that irritate and inflame the gums. In time, this can lead to red, swollen, and puffy gums. It can also lead to gum recession, where the gum tissue recedes from the tooth.
Poor oral hygiene is the most common cause of gingivitis. Brushing and flossing regularly can help to remove food particles, bacteria, and plaque from hard-to-reach places in the mouth. It’s also important to visit your dentist or dental hygienist for regular professional cleanings to remove tartar and plaque buildup on or around the teeth.
Other factors contributing to developing gingivitis include hormonal changes, certain medications, and smoking. People who smoke are more likely to develop gingivitis than nonsmokers because tobacco use slows healing in the mouth. Certain nutritional deficiencies, such as vitamin C (scurvy), can cause gingivitis.
In general, as people age, the chances of developing gingivitis increase. This is because as people age, the body produces less saliva, making it harder to rinse food and bacteria from the teeth and gums.
It is possible to reverse gingivitis as long as it is caught and treated early. If you have gingivitis, the first signs are usually bleeding gums during or after brushing and flossing. Occasionally, gums may bleed for no apparent reason. Talk to your dentist if you notice that your gums are red and swollen. They can recommend treatment options, such as anti-plaque rinses or a deeper cleaning called scaling and root planing.
Sometimes, the doctor may refer you to a gum disease specialist known as a periodontist. A specialist can treat advanced gum disease and restore the health of your gums. They can also perform X-rays to see how the gum disease has affected the bones of your jaw.
Gingivitis causes the irritation and redness of the gingiva (the gum tissue around your teeth) due to plaque buildup. You may also notice that your gums bleed when brushing or flossing. Your gums may also recede, which makes your teeth appear longer than they should be.
Unlike other forms of gum disease, such as periodontitis, gingivitis does not cause any permanent damage to the bones and tissues that support your teeth. But it’s still important to take gum disease seriously. Without treatment, gingivitis can lead to a much more serious infection called periodontitis, which can destroy the bone and tissue that hold your teeth in place and eventually cause tooth loss.
The most common cause of gingivitis is poor oral hygiene, which includes failing to brush at least twice daily, flossing, and receiving routine dental cleanings. In addition, smoking and certain medications can increase your risk for gingivitis. Hormonal changes like puberty, pregnancy, and monthly menstruation can make your gums more sensitive to irritants, which can also contribute to gingivitis. Finally, health conditions and treatments that decrease immunity, including HIV/AIDS, cancer, and leukemia, can all contribute to gingivitis.
Gingivitis isn’t a serious infection in and of itself, but it’s a sign that you should focus more on your oral hygiene habits. If you don’t, gingivitis can advance to more serious periodontitis, leading to tooth loss. If you’ve been diagnosed with gingivitis, follow up with your dentist to ensure your oral hygiene regimen is working. Ultimately, gingivitis is an easy and inexpensive condition to treat if caught early on. That’s why keeping up with your oral hygiene routine is so important. It can make all the difference in your oral and overall health! The good news is that gingivitis reverses if treated in time. So, being vigilant about your oral hygiene and visiting your dentist is vital! You’ll be glad you did. If you last saw your dentist a while ago, call us to schedule an appointment!
Gingivitis is usually reversible with a little effort and consistent care. If left untreated, gingivitis can lead to irreversible periodontitis, which can cause tooth loss.
Regular brushing and flossing are major keys to treatment. The goal is to remove the bacteria in plaque that causes inflammation and infection. Brushing with a soft-bristled toothbrush and fluoride toothpaste is recommended. Make sure to brush each tooth’s outer, inner, and chewing surfaces. Flossing is equally important to help get the plaque and food stuck between teeth and hard-to-reach areas.
Rinsing with a saltwater rinse can also reduce inflammation and kill the bacteria that cause gum disease. Add a teaspoon of salt to a glass of water and swish it around your mouth for 30 seconds, then spit it out and rinse with plain water. This can be done two or three times a day for best results.
People with underlying illnesses such as diabetes or immune system problems are predisposed to developing gingivitis because they have a weakened ability to fight bacteria that invade the gum tissue. Smoking, chewing tobacco, and over-consumption of alcohol can also contribute to developing gingivitis.
A dental professional can examine your teeth, gums, and mouth for signs of gingivitis. X-rays can show the pocket depth between your teeth and gums, indicating how bad the gingivitis is. A bacterial culture of the plaque can help identify specific bacterial species contributing to the inflammation.
Your dentist will advise you on how to treat your gingivitis and prevent it from progressing to more serious gum diseases. Changing what you eat, avoiding sugary foods and drinks, and visiting your hygienist for professional cleanings can all help to reverse gingivitis. The dental hygienist will be able to remove a lot more plaque than you can with a toothbrush and floss, and they are specially trained to spot the early signs of gum disease. If you cannot control your gingivitis with lifestyle and home treatments, your dentist may recommend antibiotics to control the inflammation.
Gingivitis is easy to treat and even easier to prevent. It’s important to know the risk factors for gingivitis and to ensure that you follow a good oral hygiene routine that includes brushing twice daily and flossing daily. You also want to ensure you visit your dentist and dental hygienist regularly. This will allow your hygienist to look for any signs of gingivitis and catch it before it becomes more serious.
When a person develops gingivitis, it is due to an overgrowth of bacteria that is called plaque. The gums respond to this irritant by creating an immune system response that produces red, puffy, tender, and sensitive gums that may bleed when brushed or flossed.
Gingivitis can be prevented by practicing a good oral hygiene routine, which should include brushing twice daily for at least 2 minutes each time and flossing once daily. It is also important to visit your Beaufort Dentist and hygienist regularly, especially if you have certain risk factors that increase the likelihood of developing gingivitis, such as:
Smoking/tobacco use; medications that cause dry mouth; hormone changes including pregnancy, birth control pills, and menstrual cycles; nutritional deficiencies, particularly Vitamin C; stress; and conditions or treatments that decrease immunity, such as HIV/AIDS, cancer, or leukemia.
In most cases, gingivitis is reversible and will clear up with regular visits to the dentist, proper oral hygiene at home (brushing and flossing), and mouthwash or rinses that contain anti-plaque agents. For severe cases, professional cleaning may be required to remove the plaque and tartar that has formed, and antibiotics may be recommended for more serious infections. These are usually short-term and will only be prescribed in consultation with your physician or dentist. Occasionally, surgery is necessary to remove infected tissue and to correct dental defects such as loose or misaligned teeth.
